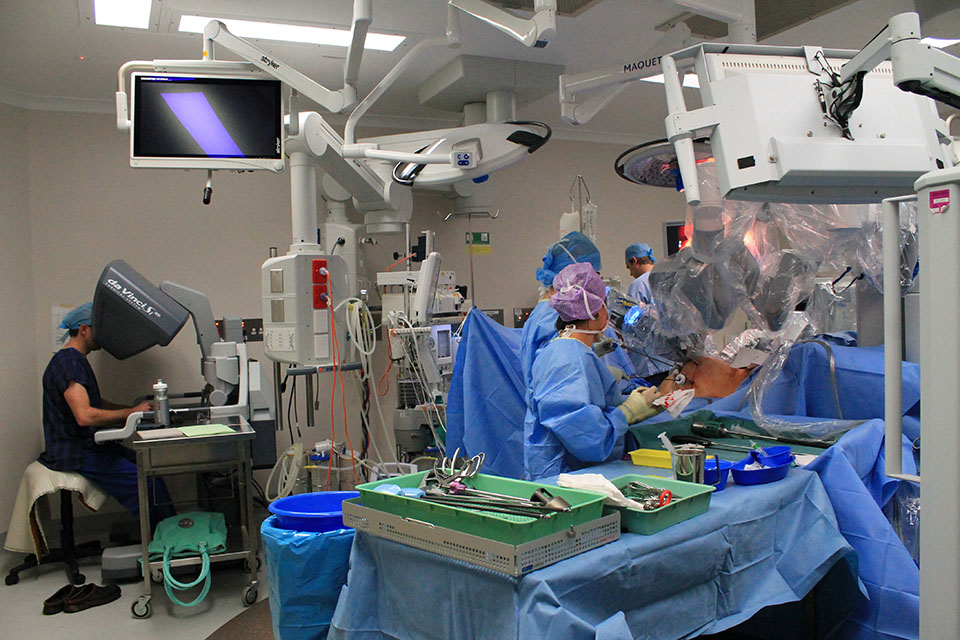
Robotic surgery giving hope to prostate cancer patients
In a world first trial, Australian researchers have found that robotic-assisted prostatectomy is providing equal outcomes for urinary and erectile function to open prostatectomy.
Published in Lancet Oncology, the study, led by researchers at Royal Brisbane and Women’s Hospital (RBWH), found that the advanced robotic technology also offered a safer and minimally invasive option for men diagnosed with prostate cancer.
Robot-assisted surgery for prostate cancer has been rapidly adopted by health professionals and is now the most widely utilised surgical approach for prostatectomy.
RBWH Urologist Dr Nigel Dunglison said the study examined surgery outcomes for around 300 Australian men over a two-year period.
“To date, very little research has been done comparing long-term outcomes of robotic-assisted prostatectomy and open prostatectomy,” Dr Dunglison said.
“Our study showed similar results for urinary and erectile function from both the robot-assisted and open surgical patient groups after 12 weeks, and these remained equal at six, 12 and 24 months.
“As technology, surgery, oncology, and radiation advances, we hope this will help improve long-term side effects experienced by prostate cancer survivors to reduce the burden of the disease on those diagnosed.
“This study has given us vital insight into the two surgical options, and will help shape further research going forward.
“We recommend that funding organisations, health care institutions and practitioners embrace minimally invasive technologies, and high-quality training is provided for surgeons to ensure patients receive the best form of care.”
Dr Dunglison said the study indicated men who underwent a robotic prostatectomy had a lower biochemical PSA recurrence after two years, however, the reason for this was not specifically studied and more research is needed to understand why.
Griffith University’s Menzies Health Institute Queensland Director Professor Suzanne Chambers said one in five participants reported elevated psychological distress 24 months after surgery.
“Unexpectedly, the study also showed that psychological distress remained high for one in five men throughout the study period and was not influenced by surgery type,” Prof Chambers said.
“These findings highlight the need for improved distress screening and psychological care long after treatment ends. “
Prostate cancer was the most common cancer diagnosed in men in Australia. Around 18,300 men are diagnosed with prostate cancer every year in Australia, and about 3200 die from the disease.
“Many patients experience long-term complications post-surgery, including reduced urinary and bowel control, erectile dysfunction and elevated psychological distress.
The study was funded by Cancer Council Queensland and undertaken by the Department of Urology at RBWH, Menzies Health Institute Queensland, and University of Queensland Centre for Clinical Research with support from the Urological Society of Australia and New Zealand.